Meet some of St George's alumni
View all Close all
By Juulia Ahvensalmi. This text was originally published as 'From the archives: International students at St George's', St George's Library Blog, 16 Jun 2021.
St George’s Medical School was formally established in 1834, but the hospital, which was opened in 1733, took pupils long before that. There were also several anatomical schools closely associated with the St George’s, including John Hunter’s Great Windmill Street school (established by John’s brother William Hunter in 1745), and Samuel Lane’s School of Anatomy and Medicine adjoining St George’s Hospital; John Hunter was a surgeon at St George’s, and Lane had also studied at St George’s.
There were fees to pay, and students could study for various lengths of time. The early student records show that some students only enrolled for a three-month period, others for six or 12 months. Initially pupils were assigned to a particular surgeon or physician. To become a perpetual pupil, there was an additional fee (which in 1870 was 100 guineas), and allowed the student admission to the practice of the physicians and surgeons of the hospital and all the lectures, allowing them to compete for any prizes and to become clinical clerks and dressers. The high fees then (as now) meant that education was not available for everyone, and the majority of the students were from the upper middle classes; many had gone to public schools and Cambridge or Oxford before attending St George’s.
 Student register 1805, showing students enrolled for various lengths of time under different surgeons. Register of Pupils and House Officers 1756-1837, SGHMS/4/1/16, Archives & Special Collections, St George’s, University of London; and Extract from student register, 1945, showing the schools and colleges attended by student prior to their enrolment at St George’s. Register of Pupils 1837-1946, SGHMS/4/1/18, Archives & Special Collections, St George’s, University of London.
Student register 1805, showing students enrolled for various lengths of time under different surgeons. Register of Pupils and House Officers 1756-1837, SGHMS/4/1/16, Archives & Special Collections, St George’s, University of London; and Extract from student register, 1945, showing the schools and colleges attended by student prior to their enrolment at St George’s. Register of Pupils 1837-1946, SGHMS/4/1/18, Archives & Special Collections, St George’s, University of London.
International connections
The student records held in the archives reveal a steady trickle of international students, based on their names (which in these early records is often the only information recorded). Names, of course, can only be used as a starting point, but the records also occasionally explicitly refer to visiting students, as in the case of Michal Astrashapovitch and Stephen Koniwetsky, who paid £20 to study under Everard Home and attend the lectures ‘for an uncertain time, to be settled at their leaving England’. There is no more information about them, but they may have been Russian – there are several other Russian names which suggests some regular contact or connection.
 Student register 1808, showing enrolment of Michal Astrashapovitch and Stephen Koniwetsky. SGHMS/4/1/16, Archives & Special Collections, St George’s, University of London.
Student register 1808, showing enrolment of Michal Astrashapovitch and Stephen Koniwetsky. SGHMS/4/1/16, Archives & Special Collections, St George’s, University of London.
Another early student was Philip Syng Physick, who had graduated from the University of Pennsylvania, and travelled to England to study under John Hunter in 1785. Known as the ‘father of American surgery’, he is said to have performed the first human blood transfusion, and was particularly interested in using autopsy as a method for observation and discovery – a practice that we can time and again see in our post mortem records.
Swedish names also appear in the registers with some regularity, especially in the 1890s when it appears to have been somewhat of a trend to travel to London to study medicine. These students include Henning Grenander, who later gained fame as a figure skater, winning the world title at the National Skating Palace in London in 1898.
 Henning Grenander. Image: skateguard1.blogspot.com
Henning Grenander. Image: skateguard1.blogspot.com
Henrik Kellgren’s ‘Swedish Institution for the Cure of Diseases by Manual Treatment’in Eton Square, London appears to have further encouraged Swedish students to study in London: Axel Wolter Louis Stackelberg, who was a pupil at Kellgren’s institute, for instance, is enrolled for 6 months as a student of anatomy in 1897, while both Kellgren’s sons Ernst and Jonas also studied at St George’s for a period; Jonas went on to study rheumatism, was a pioneer in the study of physiology of pain, and became a professor of rheumatology in Manchester in 1953.
The adventures of Hajji Baba of Ispahan
Hajee Baba may have been the first Muslim student at St George’s, and one of the first Iranian medical practitioners to study in Europe in this period. He came to England to study medicine alongside another young Iranian, Muhammad Kazim or Mohammed Cassim, in 1811 with the British ambassador to Iran, Sir Harford Jones. Hajee Baba was the son of an officer in the Shah’s army, and the sending of students to study in Britain was seen as a way of strengthening the diplomatic ties and connections between the countries; his brother trained as a mining engineer in Russia. Kazim was to study arts, but died shortly after their arrival in England.
Hajee Baba stayed in England for eight years. Following his studies, he returned to Iran to work as a physician in the court in Teheran, and in 1835 he is described as ‘a respectable elderly looking man’. He also worked as an interpreter for Persian missions abroad. Eventually he became the chief physician to the shah. He died in 1842 or 1843.
 Student register 1817, Register of Pupils and House Officers 1756-1837, SGHMS/4/1/16, Archives & Special Collections, St George’s, University of London; Cover of ‘The Adventures of Hajji Baba of Ispahan’ (1824-28) by James Justinian Morier; Poster for ‘The Adventures of Hajji Baba’ (1954), Wikipedia, ©20th Century Studios.
Student register 1817, Register of Pupils and House Officers 1756-1837, SGHMS/4/1/16, Archives & Special Collections, St George’s, University of London; Cover of ‘The Adventures of Hajji Baba of Ispahan’ (1824-28) by James Justinian Morier; Poster for ‘The Adventures of Hajji Baba’ (1954), Wikipedia, ©20th Century Studios.
He may have been the inspiration for a series of best-selling novels, ‘The Adventures of Hajji Baba of Ispahan’ (1824-28) by James Justinian Morier, secretary to Sir Harford Jones; Hajee Baba was reportedly annoyed at Morier’s use of his name for this purpose (and would have been, we can imagine, even more annoyed by the American adventure film of the same name of 1954!). Nile Green’s book ‘The Love of Strangers: What Six Muslim Students Learned in Jane Austen’s England’ (2016) recounts the story of a group of six students who travelled to Britain in 1815, based on contemporary diaries and letters of the students, in which he also mentions Hajee Baba and his unfortunate companion.
The problem of sources…
Often, the spelling of names varies considerably in different sources (this is of course particularly true when the original is in a different script), which can make tracking people difficult (but we do enjoy a bit of detective work!); there is a Wikipedia entry for Hajee Baba, for instance, but in that his name is spelled Hadji Baba Ashfar, whilst the Encyclopaedia Iranica uses the form Ḥājjī Bābā Afšār; in Persian his name is افشار، حاجی بابا.
Many students are also entered in the registers only by their first initial and surname, making identification even more problematic. A ‘foreign-sounding’ name, moreover, is of course not solid evidence either way – the somewhat exotic-sounding Peregrine Fernandez in 1799, for instance, ‘gentleman of Widcombe, Somerset’, may have had family roots elsewhere, but was born and bred in London. Where the student records are simply lists of names, as the earlier ones are, we have to turn to other sources to find out more about the people behind the names.
 Image of Assaad Y. Kayat. Source: ‘A Voice from Lebanon with the Life and Travels of Assaad Y. Kayat’ (1847).
Image of Assaad Y. Kayat. Source: ‘A Voice from Lebanon with the Life and Travels of Assaad Y. Kayat’ (1847).
One student we do know more about is Assaad Kayat, who enrolled as a student at St George’s in 1843, studying alongside Henry Gray (of Gray’s Anatomy). His fascinating story is recounted in more detail in an earlier blogpost, and his autobiography tells us a lot about his childhood in Beirut, as well as his and his wife’s experiences as immigrants in London.
The archives also reveal the story of Boghos Baghdasan Tahmisian, who, according to an appeal launched in 1892 by the Turkish Mission’s Aid Society, was a ‘native of Cilicia’, in present-day Turkey; his name may suggest Armenian origins. He is in the appeal described as a diligent student, who had arrived in London in 1889 and enrolled as a medical student at St George’s. He had, however, found himself lacking adequate funds to be able to finish his studies, which is why the society decided to appeal to the public on his behalf.
 ‘An appeal on behalf of Mr B.B. Tahmisian’ (1892) and a letter signed by Tahmisian. Archives and Special Collections, St George’s, University of London.
‘An appeal on behalf of Mr B.B. Tahmisian’ (1892) and a letter signed by Tahmisian. Archives and Special Collections, St George’s, University of London.
Pictorial propaganda
Following the end of the First World War, the Universities Bureau of the British Empire (now Association of Commonwealth Universities), established in 1913, encouraged British universities to admit students, and the Foreign Office was eager to distribute what they called ‘pictorial propaganda’:
‘The idea is to endeavour to impress the peoples of Russia and of the East with the greatness of the educational system of the British Empire’
 Letters to the Medical School, preserved in the minute books. Minutes of the Medical School Committee XII-XIII, SGHMS/1/1/1/15. Archives and Special Collections, St George’s, University of London.
Letters to the Medical School, preserved in the minute books. Minutes of the Medical School Committee XII-XIII, SGHMS/1/1/1/15. Archives and Special Collections, St George’s, University of London.
‘This medical school is unable to admit any Ceylonese students’
(Medical School minute books, 1920)
The minute books of the medical school from that time contain frequent references to the admission (or not, as it were) of international students; the minutes refer to students by their nationalities: ‘a Pole’, ‘the Siamese doctor’, ‘a native of India’.
At times, certain nationalities were the subject of intense conversations. Following the end of the First World War and demobilisation, many ‘American and colonial’ soldiers found themselves with some time to spare, and willing to use that time to study. A letter from the Royal Society of Medicine in 1918 warns that if plans to offer brief post-graduate courses for such students are not soon put in place, ‘the chances are that the majority of them will go to Paris, where […] post-graduate courses have been arranged for all Allied Officers and are already in full swing!’. The response from St George’s was not enthusiastic due to staff shortages and bureaucratic burden on the school. In the end, however, it was decided that up to 10 American students could be admitted for a three-month course, with a fee of ten guineas.
Appeals from the Egyptian Educational Mission received an even less favourable response: despite admitting two Egyptian students for a clinical course, ‘it was decided that this School cannot bind itself to admit any definite number of Egyptians’, the dean at this time wrote, suggesting that the school is too small to admit ‘foreign students […] although I am doubtful whether they ever really amalgamate or attempt to settle down with their fellow-students’.
At the moment we’re looking forward to delving into our nursing records and learning more about the student nurses at St George’s. Our initial research suggests that in the 1950s-1960s for instance up to 70% of the nursing students were immigrants to the UK; among these are many from the Windrush generation, and students came from all over the world, including the Caribbean, Ireland, India, Nigeria, Sweden and Bermuda.
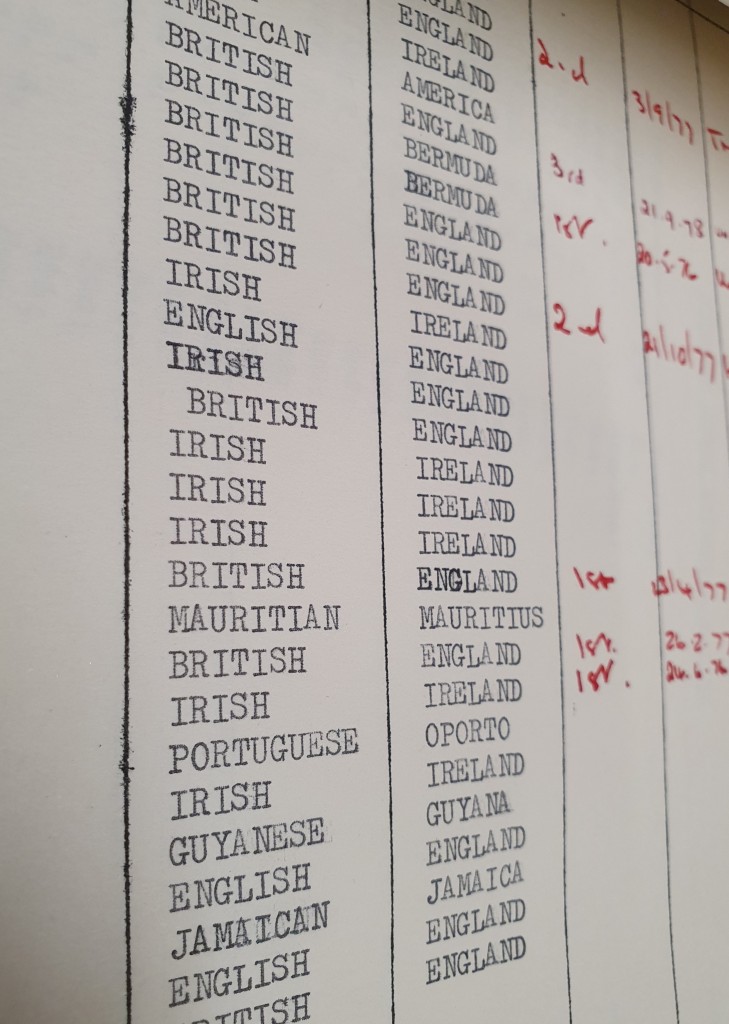 Records of nursing students at St George’s in the 1970s. Archives and Special Collections, St George’s, University of London.
Records of nursing students at St George’s in the 1970s. Archives and Special Collections, St George’s, University of London.
Want to know more, or see and study the records for yourself? Just get in touch with us at archives@sgul.ac.uk – we’d be very happy to hear from you!
The photograph below shows the dissecting room at St George’s in 1860, with lecturers and students. We know it was taken on the camera of one of the students in the picture, and Henry Gray (who wrote Gray’s Anatomy with his fellow student Henry Vandyke Carter) is depicted in the front row centre-left. On the foreground are exhibited a skull and a pair of legs. An article in St George's Gazette tells us more about the people in the photograph.
By Natasha Shillingford. This text was originally published as 'View of the Dissecting Room of St George's Hospital', St George's Library blog, 29 Jun 2020.
 View of the Dissecting Room of St George’s Hospital, Archives and Special Collections, St George’s, University of London
View of the Dissecting Room of St George’s Hospital, Archives and Special Collections, St George’s, University of London
“At the time of which I am writing, between the years 1858 and 1860, Mr Pollock and Mr Gray were Lecturers on Anatomy, Mr Athol Johnstone was Lecturer on Physiology, and Dr Noad, Lecturer on Chemistry; whilst Dr Dickinson and Dr Hastings were Demonstrators of Anatomy. All these appear in the photograph.”
‘The Men of my Time’, St George’s Hospital and Medical School Gazette, No. 3, Vol 1
George Pollock
 Photo credit: St George’s, University of London
Photo credit: St George’s, University of London
George David Pollock was born in India in 1817, the son of Field-Marshall Sir George Pollock and his wife Frances Webbe. Pollock was sent to England as a child and later apprenticed to a country practitioner. He then entered St George’s Hospital and became House Surgeon to Sir Benjamin Brodie. Due to Brodie’s influence, Pollock in 1843 gained the post of Resident Physician to Lord Metcalfe, Governor-General of Canada. Following Lord Metcalfe’s death, Pollock returned to England and in 1846 he was elected Assistant Surgeon to St George’s Hospital, where he served for thirty four years until his retirement in 1880
In 1869, the Swiss surgeon Jacques-Louis Reverdin developed a successful method for the allograft of human skin. Based upon Reverdin’s work, Pollock performed the first such successful operation in England in May 1870. This technique was known as the Pollock Graft and was adopted by many surgeons.
Pollock took over the care of ophthalmic cases at St George’s. He was also Demonstrator of Anatomy under Prescott Gardner Hewett, and succeeded him as Lecturer on Anatomy. In the Ophthalmic Department at St George’s Hospital, he was known for his cataract operations which led to his private practice in eye diseases. He was also appointed Surgeon on the founding of the Hospital for Sick Children in Great Ormond Street and took great interest in cleft palate operations.
Pollock also served as Examiner in Surgery to the Indian Medical Service where he was said to be a popular member of the teaching staff. He was also President of the Association of Fellows and headed a reform party at the Royal College of Surgeons. He was President of the Royal Medico-Chirurgical Society in 1886, and of the Pathological Society in 1875, and also Surgeon in Ordinary to the Prince of Wales.
He practiced at 36 Grosvenor Street until the last year of his life, when he moved to 35 Chester Square. He married Marianne, daughter of Robert Saunders, in 1850 by whom he had five children, three surviving him. He died on 14th February 1897 after a short illness of pneumonia.
Henry Gray
 Copyright expired. CC BY 4.0
Copyright expired. CC BY 4.0
Henry Gray was born in 1827, the son of a Private Messenger to George IV and William IV. He entered St George’s Hospital on 6th May 1845 and he soon focussed his attention on the study of anatomy. In 1848, at the age of 21, he was awarded the Triennial Prize of the Royal College of Surgeons for his essay on ‘The Origin, Connection and Distribution of the Nerves of the Human Eye and its Appendages, illustrated by Comparative Dissections of the Eye in other Vertebrate Animals’. As a student he was described as a painstaking and methodical worker who learned anatomy by undertaking dissections himself.
In 1850 Gray was appointed House Surgeon under Robert Keate, Caesar Hawkins, Edward Cutler and Thomas Turner. On 3rd June 1852 he was elected a Fellow of the Royal Society, a rare distinction at the age of 25. Gray devoted himself to the study of anatomy and the first edition of his ‘Anatomy, Descriptive and Surgical’ was published in 1858, with engravings by Dr Henry Vandyke Carter. The book, known as ‘Gray’s Anatomy’, had reached the 23rd edition by 1928.
In 1861, Gray became a candidate for the post of Assistant Surgeon at St George’s Hospital. His election was viewed to be certain, but he contracted smallpox while looking after a nephew with the disease, and died after a short illness on 13th June 1861. Upon his death, Sir Benjamin Brodie wrote ‘I am most grieved about poor Gray. His death, just as he was on the point of realizing the reward of his labours, is a sad event indeed…Gray is a great loss to the Hospital and the School. Who is there to take his place?’
Athol Archibald Wood Johnstone
 Post Mortem examination book 1844 (Anne Thompson, PM/1844/64) Archive and Special Collections, St George’s, University of London
Post Mortem examination book 1844 (Anne Thompson, PM/1844/64) Archive and Special Collections, St George’s, University of London
Athol Archibald Wood Johnstone was born in 1820, the youngest son of Dr James Johnson, Physician to King William IV, whose name was accidentally spelt Johnson instead of Johnstone. Athol Johnstone reverted to the original family name on the death of his father.
He studied at St George’s Hospital, where he became House Surgeon, Demonstrator of Anatomy and Lecturer on Physiology. He later succeeded George Pollock as Surgeon to the Hospital for Sick Children, Great Ormond Street. Johnstone was also Surgeon to the Royal Alexandra Hospital for Children with Hip Disease, and to St George’s and St James’s Dispensary. In 1861 he declined to stand for the vacancy of Assistant Surgeon to St George’s Hospital following the death of Henry Gray. In 1862 he moved to Brighton where he practiced as Surgeon to the Brighton and Sussex Throat and Ear Hospital, the Invalid Gentlewomen’s Home, and the Brighton Battery of the old Royal Naval Artillery.
He was twice married, his second wife surviving him. Johnstone died on 16th March 1902 in Brighton.
Henry Minchin Noad
Henry Minchin Noad was born in 22nd June 1815 at Shawford, Somerset, the son of Humprey Noad. He was educated at Frome Grammar School. He began the study of chemistry and electricity, and about 1836 he delivered lectures on both subjects at the literary and scientific institutions of Bath and Bristol. He joined the London Electrical Society in 1837.
In 1845 he began his studies under August Wilhelm Hofmann at the Royal College of Chemistry. He joined the medical school of St George’s Hospital in 1847 when he was appointed to the chair of Chemistry. He remained in this role until his death.
In 1849 Noad obtained his degree of doctor of Physics from the University of Giessen. In 1850-51 he conducted an inquiry into the composition and functions of the spleen with Henry Gray. In 1856 he was elected a Fellow of the Royal Society. He was appointed Consulting Chemist to the Ebbw Vale Iron Company, the Cwm Celyn, and Blaenau, the Aberdar and Plymouth, and other iron works in South Wales. In 1866 he became an examiner of malt liquors at the India Office. In 1872 he became an examiner in Chemistry and Physics at the Royal Military Academy in Woolwich.
Noad died at his home in Lower Norwood, London on 23rd July 1877, survived by his wife Charlotte Jane.
William Howship Dickinson
 Image in public domain
Image in public domain
William Howship Dickinson was born on 9th June 1832 in Brighton, the son of William Dickinson of Brockenhurst. He was educated at Caius College, Cambridge and at St George’s Hospital. After graduating in 1859, he became Curator of the Museum, Assistant Physician in 1866 and Physician in 1874. He was also Assistant Physician from 1861 to 1869 at the Hospital for Sick Children, and later physician from 1869 to 1874. He held the offices of Censor and Curator of the Museum at the Royal College of Physicians, delivered the Croonian Lectures in 1883 and the Harveian Oration in 1891. Dickinson was Examiner in medicine to the Royal College of Surgeons and to the Universities of Cambridge, London and Durham.
Thomas Pickering Pick recalled attending an anatomy demonstration by William Howship Dickinson. He said that ‘The first of these which I attended was on the kidney, and a specimen from the dead-house was exhibited. I ventured to ask, no doubt with all diffidence as a beginner, whether it was not a very large one, and was met by the remark: “By no means; perhaps you are thinking of the kidneys you have eaten for breakfast this morning.” At this there was a universal titter, and I felt extremely small. But undoubtedly the suggestion was a perfectly true one. It was the first time I had seen a human kidney, and my knowledge of that particular organ was entirely derived from the sheep’s kidney on the breakfast table.’ (‘The Men of my Time’, St George’s Hospital and Medical School Gazette, No. 3, Vol 1)
Dickinson was a general physician but he was known as an authority on diseases of the kidney and children’s diseases. He was known to be a meticulously careful observer who visited the wards of St George’s Hospital every day to observe his patients and take their medical histories. Dickinson was said to have ‘worshipped St George’s Hospital almost to the point of idolatry and received in return, during his long life, no small measure of its homage.’
In 1861 he married Laura, daughter of James Arthur Wilson, physician to St George’s Hospital. They had four daughters and two sons. Dickinson died on 9th January 1913.
Cecil Hastings
Unfortunately not much is known about Dr Cecil William Hastings, Demonstrator of Anatomy at St George’s Hospital. The student registers of the medical school reveal that he was educated at the University of Oxford and became a Member of the Royal College of Physicians. He took the post of House Surgeon in 1853 and was also Physician at the Royal Pimlico Dispensary.
Search the Authority Records on the Archives and Special Collections catalogue to find out more about the Surgeons and Physicians of St. George’s Hospital (https://archives.sgul.ac.uk/).
One of St George's most famous alumni is Edward Jenner, who is credited with developing smallpox vaccination in the 1790s, which eventually, in 1976, led to the eradication of smallpox. Vaccination (or inoculation) as such was not a new invention: Jenner's innovation was to use the related, but much less dangerous, cowpox. The famous cow who helped him in this endeavour was called Blossom, and her hide is still displayed at the SGUL Library.
The archive holds a manuscript letter written by Jenner in 1807, and the volumes in which he laid out his arguments, including
- Causes and Effects of Variolae Vaccinae, 1798 (inscribed by Jenner)
- The Origin of the Vaccine Inoculation, 1801

John Hunter, often referred to as the 'founder of scientific surgery', was a student and surgeon at St George's. His legacy is nowadays quite controversial - although his contributions to medicine and anatomy are impressive, his methods in acquiring specimens were often cruel.
The archive holds correspondence by and to John Hunter, as well as various books written by him, including 'A Treatise on the Venereal Disease' (1786) and 'A Treatise on the Blood, Inflammation and Gun-Shot Wounds' (1794).
Charles Byrne, known as the 'Irish Giant' suffered from acromegalic gigantism, and before his untimely death at the age of 22 left behind explicit instructions to not let Hunter have his body. His skeleton (whose legs are pictured on the wall in the image below), however, is still preserved at the Hunterian Museum in London, although there is debate of what should be done with his remains. Hunter died during a meeting at St George's, and his couch and table are displayed in the lobby.

By Juulia Ahvensalmi. This text was originally published as 'Former students of St George's: Assaad Y. Kayat (1843-1846)', St George's Library blog, 18 Aug 2020.
 Image of Assaad Y. Kayat. Source: ‘A Voice from Lebanon with the Life and Travels of Assaad Y. Kayat’ (1847).
Image of Assaad Y. Kayat. Source: ‘A Voice from Lebanon with the Life and Travels of Assaad Y. Kayat’ (1847).
Going through student records recently in the archives, I came across the name Assaad y Kayat in the list of students enrolled at St George’s in 1843. There was not much information in this list: his student number was 4093, he had attended the medical school for three seasons and he ‘appears not to have paid his fees’. His name stood out from the list of predominantly British names (the students at St George’s were until relatively recently primarily white, middle or upper class and male – you can read about our first female studnets in 1915 here), but the brief description was also intriguing. Who was Assaad, where did he come from and what happened to him?
As luck would have it, it turns out that Assaad, helpfully for us, published a book with his life story. He spelled his name As’ad Yakub Khayyat or Assaad Y. Kayat, and the book he wrote was called ‘A Voice from Lebanon, with the Life and Travels of Assaad Y. Kayat’. It was originally published by Madden & Co on Leadenhall Street, London, in 1847, and the front page includes a (rather dashing) portrait of him (see above).
The book appears to have been written specifically for a British audience. He had spent time in England on three occasions: it was on his third trip that he became a student at St George’s. At the age of 32 when he began his studies, he would have been considerably older than most of his fellow students – Henry Gray, for instance, was only 16 when he began his studies the previous year. Assaad was also married and had two small children, and had to earn money to cover his studies, so he presumably did not have much time for student activities. In his book, however, he only has words of praise for his time as a student:
‘I … entered as a medical student at St George’s Hospital … I shall be for ever indebted to them for the instruction I have received from their high skill. It is indeed a glorious hospital, an exalted medical school; it is an honour to be taught at it’
 Signature of Assaad Y. Kayat in the St George’s Hospital Medical School Register 1836-1902. Archives and Special Collections of St George’s, University of London
Signature of Assaad Y. Kayat in the St George’s Hospital Medical School Register 1836-1902. Archives and Special Collections of St George’s, University of London
Life and travels of Assaad Y. Kayat
Born in 1811 in Beirut, Assaad describes in vivid detail his childhood and upbringing, through epidemics, wars and revolutions. He learns to read and write at the age of four, first in Arabic, his mother tongue, as his father wants to give him a good education (‘from the fear of my growing to manhood in a state of wretchedness and oppression’). Showing great promise and inclination for learning languages (he subsequently learns both ancient and modern Greek, Italian, English and Persian) as well as an astute business sense, Assaad soon progresses from selling rag papers to interpreting for sailors and merchants and is eventually employed as an interpreter by the British consul and representative of the East India Company in Syria. He travels widely around Middle East and Europe. Keeping in mind his audience, there is a lot of name-dropping of British dignitaries, officials and other people he meets on the way – his skills at networking are clearly second to none.
Although his focus is on Christian missionary activities, his account comes across as strikingly liberal for its time: he talks of ‘native agency’ and the importance of having native teachers and preachers, as well as of learning local languages and customs. He is a keen advocate of education, and in particular women’s education and equality.
Medical education
Throughout the account, he emphasises his journey to become a doctor ‘in order to benefit my fellow creatures’. On his second visit to England in the later 1830s, he attends some medical lectures at Cambridge, as well as at St George’s, where his first connection appears to have been the hospital chaplain, Rev William Niven. He regards medical education as an essential:
‘It requires no miracle to heal, but only to attend a medical course for a diploma or degree. A dose or two of sulphate of quinine often cures your patient of ague; vaccination prevents his taking the small-pox; the use of certain precautions prevents your catching the plague.’
In 1843 he returns to England, accompanied by his wife and toddler, as well as a group of young men with the view of obtaining an education for them, and to study medicine at St George’s. It is not all plain sailing, however, His wife Martha struggles to settle in; she has a toddler and a small baby to care for, she is sick herself, cannot get used to the miserable weather and the famous London fogs (or smogs caused by pollution in the dirty and overcrowded city), she doesn’t speak English and is largely confined to their small rented rooms, instead of their lovely house and garden and the company of her family and friends in Beirut (so despite his advocacy for women’s education, his own wife is stuck with a very traditional role at home). They are struggling with money; the committee (‘Committee of the Syrian Society’) Assaad had set up to enable the education for his ‘Syrian youths’ is slow to help, and Assaad attempts to raise money by giving public lectures on Syria and Christianity and by setting up a small importing and exporting business.
He is also keenly aware of his status as an immigrant in Britain and encounters prejudices and racism. He cites a journalist, who ‘came to my lectures twice, and all she could observe was my handsome appearance – her ears tickled by my foreign accent’ and talks at length about the difficulties in trying to expel these prejudices:
‘Some take me for a prince, or at least a chief; others, for a Chinese ambassador, a merchant, or an interpreter. Some think I am a Jew; others, a Turk, a missionary, a philosopher, or a lecturer; Christians of every denomination appointing to me a station or an office according to their own preconceived notions.’
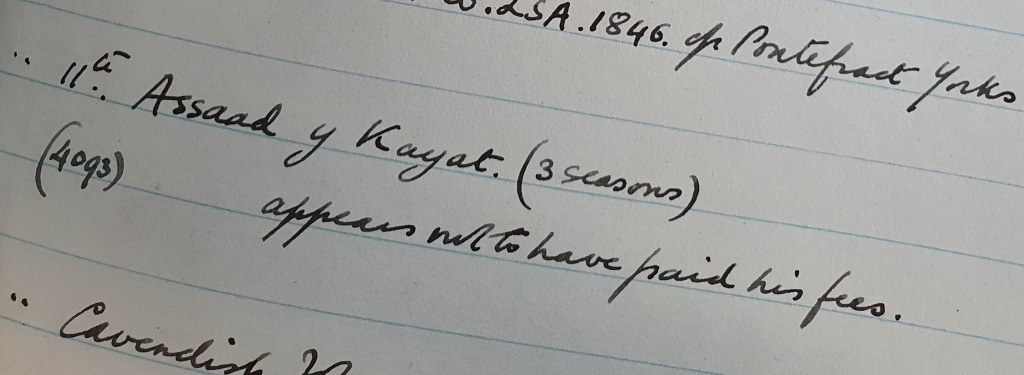 Entry for Assaad Y Kayat (student number 4093). St George’s student records Vol 5. SGHMS/4/1/7. Archives and Special Collections of St George’s, University of London.
Entry for Assaad Y Kayat (student number 4093). St George’s student records Vol 5. SGHMS/4/1/7. Archives and Special Collections of St George’s, University of London.
The student records show that Assaad studied for three seasons. One of the records notes that he ‘appears not to have paid his fees’, but according to his own account he finishes his studies in 1846, obtains his diploma and is admitted as a member of the Royal College of Surgeons, before returning to Beirut. It is unclear which account is true; maybe some more research in the archives will shed more light on the matter.
Helen Ingleby was one of the first female students at St George's in 1915, the first time women were admitted as medical students. She began her studies alongside three other women, Hetty Ethelberta Claremont, Marian Bostock and Elizabeth O'Flynn.
After qualifying, she worked at St George's as the curator of the Pathological Museum, medical registrar and house physician. She performed many post mortems during her time at St George's.
After the First World War ended, St George's decided that there was no more space for female students or doctors, and the contracts of those who remained were terminated by the early 1920s. Ingleby went on to work at the Victoria Hospital for children and the South London Hospital for Women. She lectured on pathology at King's College Hospital, and received a fellowship to study at the Johns Hopkins, University of Baltimore. She stayed in Philadelphia, working at the Women's Hospital and becoming a professor at the Albert Einstein Medical Centre. She finally received her MD in 1954, almost 40 years after first qualifying as a doctor.
In this photograph Helen Ingleby is pictured on the left; the other woman in the photograph is her fellow student Hetty Ethelberta Claremont.

Norah Schuster studied medicine at the University of Manchester, qualifying in 1918. She moved to London, where she was employed at St George's, initially as an unpaid house physician to the neurologist James Collier in 1920, and later as an assistant pathologist. She also worked in the Pathological Museum, including updating the specimen catalogues and performed post mortems until at least 1929 at St George's.
She was the last woman to be employed in a clinical role at St George's until after the Second World War, when women were again allowed to enrol as medical students. The archive holds her memoir, 'A clinical pathologist day by day 1916-1960' and an oral history interview, recorded in 1989 when she was 97 years old.

By Juulia Ahvensalmi. This text was originally published as 'Former students of St George's: Kathryn Hamill Cohen (1905-1960)', St George's Library blog, 5 Oct 2020.
 ‘Death of a Ziegfeld girl’, The Daily Mail, 5 Jan 1960. Source: Patricia Highsmith Papers, Swiss Literary Archives.
‘Death of a Ziegfeld girl’, The Daily Mail, 5 Jan 1960. Source: Patricia Highsmith Papers, Swiss Literary Archives.
Newspaper headlines in 1960 made much of the death of Kathryn Hamill Cohen. Portrayed looking elegant and glamorous, newspaper reports could hardly contain themselves – the story, after all, seemed to have it all: suicide of a Chelsea doctor, psychoanalyst and a Broadway dancer. She was also a lover of Patricia Highsmith. But who was she, and what was her connection to St George’s?
Kathryn Hamill Cohen was one of the first female students to enter the Medical School when St George’s again admitted women in 1945, for the first time since the First World War. There had been considerable resistance to the idea of female students, and it was only in 1915 that first female students were admitted to St George’s. Even then, their time was limited, and after the war the doors of the medical school were again closed to women.
 University of London, Report of Special Committee on Medical Education of Women, 1944. Medical School Committee Minutes, Vol 26, SGHMS/1/1/1/29, Archives and Special Collections, St George’s, University of London.
University of London, Report of Special Committee on Medical Education of Women, 1944. Medical School Committee Minutes, Vol 26, SGHMS/1/1/1/29, Archives and Special Collections, St George’s, University of London.
The minutes of the Medical School show that co-education (that is, women and men studying together) was a hotly debated subject between the wars, and St George’s also received petitions and requests to allow women to continue studying alongside men. Progress was, however, slow, and so it was not until 1944 that a report by the London universities found that, in fact, patients (astonishingly) did not mind being examined by female students, and since opposition to co-education appeared to be diminishing and many universities were already admitting women, the remaining argument against allowing female students appeared to be that ‘the Schools for men are loath to lose their traditions which have been built up by generations of male students’.
 Student register 1945 showing the first female students at St George’s since the First World War. SGHMS/4/1/18, Archives and Special Collections, St George’s, University of London.
Student register 1945 showing the first female students at St George’s since the First World War. SGHMS/4/1/18, Archives and Special Collections, St George’s, University of London.
And so Cohen was admitted to study at St George’s alongside with four other women in 1945: Ruth Clare Cornford (Chapman), Patience Proby, Adrien Patricia Dunlop and Zaïda Megrah (Hall / Ramsbotham). Being one of so few women must have been hard – even the student records had everything printed as ‘Mr’ as default, as Cohen’s attendance card for anaesthetics shows below. Furthermore, while the other women were in their early 20s, Cohen was 40 when she began her studies at St George’s. Her outlook on life and on her studies must have differed considerably from that of her fellow students.
 Attendance card from the Department of Anaesthetics. Student index cards A-C, Archives and Special Collections, St George’s, University of London.
Attendance card from the Department of Anaesthetics. Student index cards A-C, Archives and Special Collections, St George’s, University of London.
Prior to her medical studies, she had led an eventful life. Born in New York in 1905, she had worked as a dancer at Broadway with the Ziegfeld Follies, who were hugely successful, glitzy revue performers with elaborate choreographies.
 Ziegfeld Follies. Source: All That’s Interesting: ‘Ziegfeld Follies: The Other, Sensational Side of Flappers’, 4 Apr 2015.
Ziegfeld Follies. Source: All That’s Interesting: ‘Ziegfeld Follies: The Other, Sensational Side of Flappers’, 4 Apr 2015.
In 1930 she moved to the UK; her arrival is recorded on a passenger list from New York to Plymouth on 30 Dec 1930. She was 25 years old, and her occupation on this list is given as actress. Later that year she married Dennis Cohen, a publisher at the Cresset Press, who may have been an MI6 officer, and who was also involved in organising Kindertransport from Germany during the war. They eventually moved to Chelsea, where they had commissioned an avant-garde house still known as the ‘Cohen house’.
![Image of the so-called Cohen House at 64 Church Street, Chelsea. ©Gillfoto [aka Kenneth John Gill] CC BY-SA 3.0.](/image-library/default-images/image6-cohenhouse.jpg) Image of the so-called Cohen House at 64 Church Street, Chelsea. ©Gillfoto [aka Kenneth John Gill]CC BY-SA 3.0.
Image of the so-called Cohen House at 64 Church Street, Chelsea. ©Gillfoto [aka Kenneth John Gill]CC BY-SA 3.0.
At some point prior to 1945 Cohen worked as a secretary to Nye Bevan, who in 1948 went on to establish the NHS: perhaps this work prompted her to consider medical studies, rather than politics. Between 1941 and 1944 she was a student at Newnham College, Cambridge, where she studied anatomy, physiology and biochemistry. She enrolled as a student at St George’s in September 1945, a week after the official end of Second World War 2 September 1945.
 Student photograph of Cohen, Kathryn Hamill, 1945. Student index cards A-C, Archives and Special Collections, St George’s, University of London.
Student photograph of Cohen, Kathryn Hamill, 1945. Student index cards A-C, Archives and Special Collections, St George’s, University of London.
After graduating from the medical school in 1948, her student records show that she worked as house officer and registrar at St George’s Hospital for several years (and even in her student photograph she looks glamorous). Later she was employed as psychoanalyst at the hospital and appears to have practiced psychiatry from her home office. She was also interested in genetics, and published on the use of hypnosis in treating skin diseases. Although psychoanalysis may now have a dubitable reputation, it was a respected field of study at the time.
During this time she met the author Patricia Highsmith at a party in New York. The two had an affair in 1949: “Kathryn was beautiful, intelligent, melancholy, monied, and married: a combination Pat always found irresistible”. Highsmith asked Cohen to accompany her on a trip to Italy, although the affair does not appear to have continued after that.
 Patricia Highsmith. Source: New York Times, 25 Oct 2019, ‘The Talented Patricia Highsmith’s Private Diaries Are Going Public’.
Patricia Highsmith. Source: New York Times, 25 Oct 2019, ‘The Talented Patricia Highsmith’s Private Diaries Are Going Public’.
It was this connection to Highsmith that made Cohen famous, as she was a partial inspiration for Highsmith’s novel ‘The Price of Salt’ (later republished as ‘Carol’ and made into a film in 2015), a departure from her usual psychological thrillers in that it was a romance – and a lesbian romance at that, which in the 1950s was somewhat scandalous. Dennis Cohen’s publishing house (for which Cohen worked for as a co-director) published several of Highsmith’s books, including ‘Strangers on a Train’, which Alfred Hitchcock made into a film.
 Cate Blanchett as Carol in the 2015 film. Source: The Playlist.
Cate Blanchett as Carol in the 2015 film. Source: The Playlist.
Her life, however, had a tragic end: in 1960 Cohen took her own life by taking an overdose of barbiturates. In a further (if morbid) connection to St George’s, her post mortem was performed by Donald Teare, pathologist at St George’s, and also a former student of St George’s.