This article is part of a series of research impact stories related to our REF 2014 submission.
Professor Alicja Rudnicka is evaluating whether advanced Artificial Intelligence (AI) software can help to detect eye problems in people with diabetes and reduce the burden on national eye screening programs.
Over 400 million adults around the world are living with diabetes. 10% have Type 1 diabetes, which often needs insulin treatment from childhood. 90% have later-onset Type 2 diabetes which tends to run in families, although the age at which it starts can be influenced by bodyweight and lifestyle.
Diabetes can cause a range of complications, including eye problems known as diabetic retinopathy. This develops when poorly controlled blood sugar levels damage the blood vessels at the back of the eye, leading to sight loss and even blindness. Identifying early signs of the disease is key to providing effective treatment and preventing people with diabetes from losing their vision.
Most people with Type 1 and nearly two thirds of people with Type 2 diabetes will have some degree of diabetic eye disease within two decades of diagnosis
In the UK, people with diabetes are checked for signs of retinopathy at least once every year through a national eye screening program, where images of their eyes are examined by experts for any signs of disease. But with over 2 million eye screening appointments per year in England alone, and rapidly rising rates of diabetes, the system is becoming overwhelmed.
‘National eye screening programs for diabetic retinopathy are effective, but are labour intensive and expensive,’ says City St George’s Professor of Statistical Epidemiology, Professor Alicja Rudnicka. ‘We undertook a study examining the accuracy of AI software to detect diabetic retinopathy, to see whether we could partially replace humans with the software to screen for diabetic eye disease.’
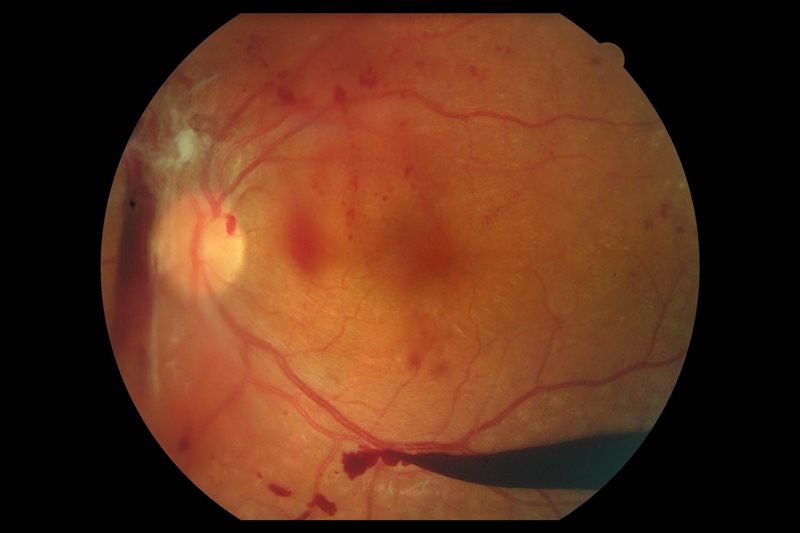 An image of the back of an eye showing signs of diabetic retinopathy.
An image of the back of an eye showing signs of diabetic retinopathy.
The study, which was funded by the National Institute for Health Research, tested the system on 20,000 patients.
‘The aim of the AI software is to identify high-risk images for further assessment by human graders,’ she explains. ‘We found that the software is extremely good at detecting images of those with diabetic retinopathy, particularly sight-threatening disease. It could reduce the workload of human graders by half, making it a very cost-effective alternative to a fully manual human grading system’.
‘We hope that the system will soon be introduced in one of our partner centres in London and that it will be rolled out across other diabetic eye screening centres within the next five years, potentially saving the NHS over £10 million per year,’ she says.
In the meantime, Rudnicka is working with Professor Christopher Owen from the Population Health Research Institute at the School of Health & Medical Sciences and colleagues at Moorfields Eye Hospital and the Homerton University Hospital to further evaluate the performance of these AI software systems in other ‘real-life’ diabetic eye screening programmes, which they hope will lead to a change in clinical practice and widespread use of these systems throughout the NHS.